Antimicrobial chemotherapy involves using chemical agents to treat infections caused by microorganisms such as bacteria, viruses, fungi, and parasites. The discovery of antibiotics transformed medicine, enabling effective treatment of previously deadly bacterial infections. Today, however, increasing drug resistance and the diversity of pathogens have created a need for strategies that go beyond traditional antibiotics.
Antibiotics: The Foundation of Antimicrobial Therapy
Antibiotics are substances that either kill bacteria or inhibit their growth. They can be natural, semi-synthetic, or entirely synthetic. Common classifications based on their action include:
- Inhibitors of cell wall synthesis – such as penicillins and cephalosporins, which prevent bacteria from forming proper cell walls.
- Protein synthesis inhibitors – such as tetracyclines and macrolides, which disrupt bacterial ribosomes.
- Nucleic acid synthesis inhibitors – like fluoroquinolones, which interfere with DNA replication.
- Metabolic pathway inhibitors – such as sulfonamides, which block folic acid production.
Despite their life-saving potential, overuse of antibiotics has led to widespread antimicrobial resistance (AMR). Drug-resistant bacteria, including methicillin-resistant Staphylococcus aureus (MRSA) and multidrug-resistant Gram-negative strains, now pose serious therapeutic challenges
Moving Beyond Antibiotics
1. Antiviral Drugs
Viruses replicate inside host cells, so antiviral agents must target the virus without damaging the host. They work by:
- Preventing viral entry into cells.
- Inhibiting viral enzymes necessary for replication.
- Blocking viral assembly or release.
Examples include acyclovir for herpes infections and oseltamivir for influenza.
2. Antifungal and Antiparasitic Therapies
Fungal infections are increasingly common, particularly in immunocompromised individuals. Treatments like azoles, echinocandins, and amphotericin B target fungal cell membranes or walls. Similarly, antiparasitic drugs such as artemisinin disrupt essential parasite pathways.
3. Monoclonal Antibodies and Immunotherapy
Monoclonal antibodies can neutralize pathogens or their toxins. They have been developed against toxins from Clostridioides difficile and respiratory viruses. Immunotherapy can also enhance the body’s own defenses rather than directly attacking pathogens.
4. Phage Therapy
Bacteriophages, viruses that infect bacteria, offer precise treatment for antibiotic-resistant bacterial infections. Phage therapy is gaining renewed interest as a complementary or alternative approach to antibiotics, targeting harmful bacteria while sparing beneficial microbiota.
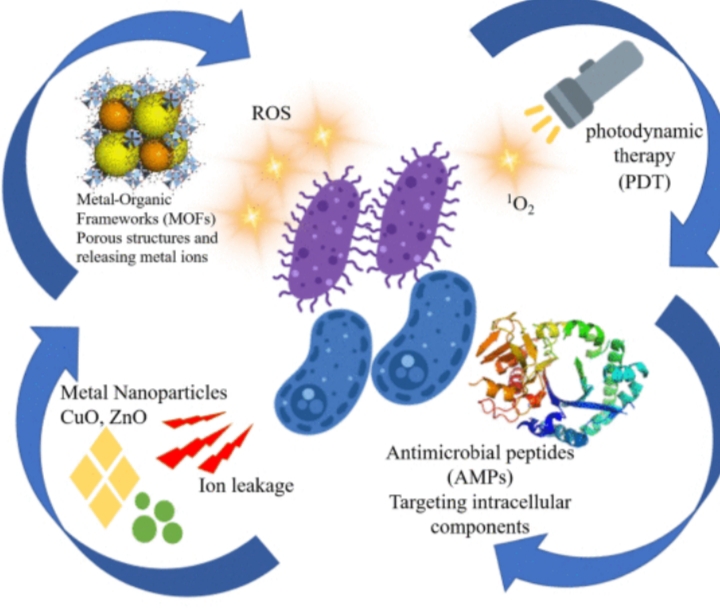
5. Novel Small Molecules and Antimicrobial Peptides
New synthetic or naturally derived molecules can disrupt microbial membranes or interfere with signaling pathways. Antimicrobial peptides show promise due to their broad-spectrum activity and lower risk of resistance development
Challenges and Future Perspectives
Key challenges in modern antimicrobial therapy include:
- Antimicrobial resistance (AMR) – projected to cause millions of deaths annually if left unchecked.
- Slow drug development – producing new antibiotics is costly and time-consuming.
- Rapid diagnostics – essential for identifying pathogens and tailoring therapy.
Conclusion
While antibiotics remain fundamental in treating infections, rising resistance demands innovative solutions. The future of antimicrobial chemotherapy involves combining traditional antibiotics with antivirals, antifungals, immunotherapies, and emerging technologies such as phage therapy. Advancing these strategies is critical to sustaining the success of modern medicine against infectious disease
